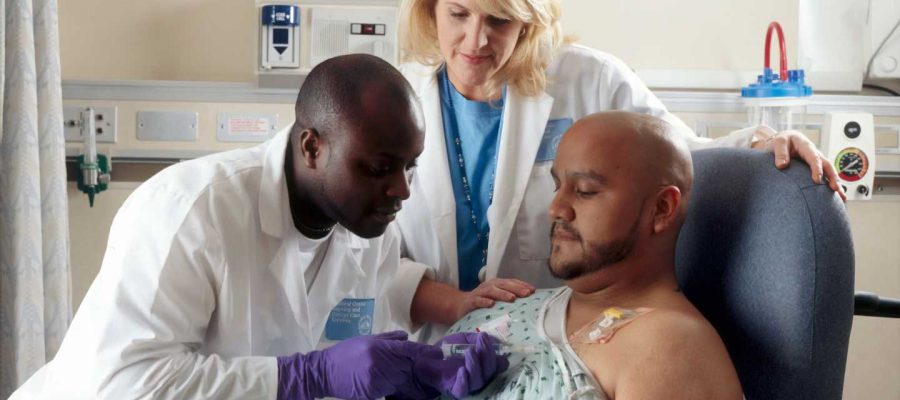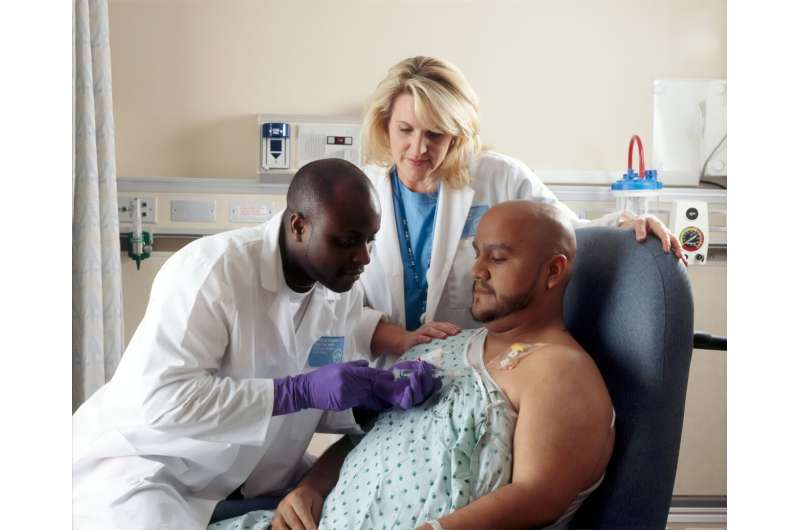
Growing up on the South Side of Chicago as the child of Mexican immigrants who primarily spoke Spanish, Dr. Daniel Meza was often asked to translate for his parents during medical appointments.
“It’s a skill that I grew up with, having that technical language,” Meza said. “I just recall how stressful it was for my parents when they were in clinics, and as well as for myself, being a small child.”
Now a pulmonologist with Northwestern Medicine, Meza says his concerns about equity in health care lingered.
Two months ago, Meza became a part of the Northwestern Medicine Canning Thoracic Institute Hispanic Program. Patients of the program receive lung and thoracic care, including surgery and preventive screenings, entirely in Spanish.
Everyone at the CTI Hispanic Program, from front desk workers to operating room nurses, is fluent in Spanish. Patients can also access a dedicated Spanish-language phone line.
Staff aim to improve health equity in Chicago by building trust with Hispanic patients and improving treatment outcomes in Hispanic communities, Meza said.
Some 28.7% of Chicagoans, or about 750,000 people, identified as Hispanic as of the 2022 census.
“When I see patients come in with their children and they see I speak Spanish, there’s kind of a relief on both sides,” Meza said.
The program launched two months ago. It is led by Dr. Diego Mauricio Avella Patino, a thoracic surgeon trained in Colombia, and by Meza, both native Spanish speakers. Avella performs surgeries related to esophageal disease, lung failure, various cancers, chest wall issues and breathing obstruction. Meza specializes in treating pulmonary problems such as asthma, respiratory failure and emphysema.
Patients are often surrounded by medical staff in their most vulnerable moments, such as right before anesthesia.
Those who can be treated in their primary language tend to forge better relationships with care providers and follow aftercare instructions better, Avella said.
“The need was overwhelming,” said Avella, who worked at Northwestern Medicine for two years before the program launched.
Patients may also feel more comfortable asking detailed questions with doctors who understand the cultural norms they experience daily, Avella said.
“Sometimes the barriers for the patients to be compliant with the recommendations are beyond the disease itself, they are social,” Avella said. “When you build that bridge with the patient, it can be extremely powerful.”
Avella said some of his patients have been treated “suboptimally” at other clinics in the past. He recently saw a lung cancer patient who suffered from extreme untreated nausea. Avella discovered that the patient had been diagnosed with diabetes, but rarely spoke of it.
“This patient was never going to get her diabetes appropriately controlled because she didn’t have a doctor who was taking care of her,” Avella said. The patient is now being treated by Northwestern Medicine endocrinologists.
Patients in the CTI Hispanic Program are often referred to other Northwestern Medicine specialists, Avella said. Program staff work with these patients to schedule and prepare for future appointments in Spanish, Avella said.
The clinic is also focused on preventive measures for respiratory issues. Proposing that patients quit smoking and get screened for lung cancer has been a priority for Meza.
“There are a lot of great medications out there that we know help increase the chances of a patient quitting,” Meza said. “And in any population we have, that’s not something they’re aware exists.”
While smoking rates in Chicago are on the decline, Meza said, he’s had to convince at least one ex-smoker to schedule a lung cancer screening. Catching lung cancer at an early stage improves patient outcomes significantly, Meza said.
The program has seen higher rates of asthma and respiratory issues among patients living in the Pilsen and Little Village neighborhoods, Meza said. He attributes this to nearby factory smoke and other forms of air pollution within the last decade.
Raising patient awareness of ongoing clinical trials is also a goal, Meza said.
The American Medical Association reported in 2022 that Hispanic patients with limited English proficiency are highly underrepresented in clinical trials, particularly for vaccines and cancer treatment. In 2019, 18.5% of the United States adult population, but only 3% of cancer clinical trial participants, identified as Hispanic.
Meza and Avella both said that while working with new patients, they’re conscious of the wide diversity among Hispanic Chicagoans.
“There are people from very different racial backgrounds, educational backgrounds, financial backgrounds and many different countries of origin,” Avella said. “What I can do right now is provide health care attention in Spanish and at least be a little more culturally aware of the differences among Hispanics.”
Support within Northwestern Medicine and among colleagues has made Chicago ideal for the program, Avella said. He hopes other cities with large Spanish-speaking populations will consider the clinic a model for similar programs.
Meza also hopes to forge more connections with smaller health clinics in neighborhoods with high concentrations of primarily Spanish-speaking residents. Many Hispanic patients, particularly those of lower socioeconomic status, start their care journeys there, he said.
“As (the CTI Hispanic Program) grows, I do hope that we are kind of like a beacon in the city for pulmonary thoracic needs in the Hispanic community,” Meza said.
2023 Chicago Tribune.
Distributed by Tribune Content Agency, LLC.
Source: Read Full Article