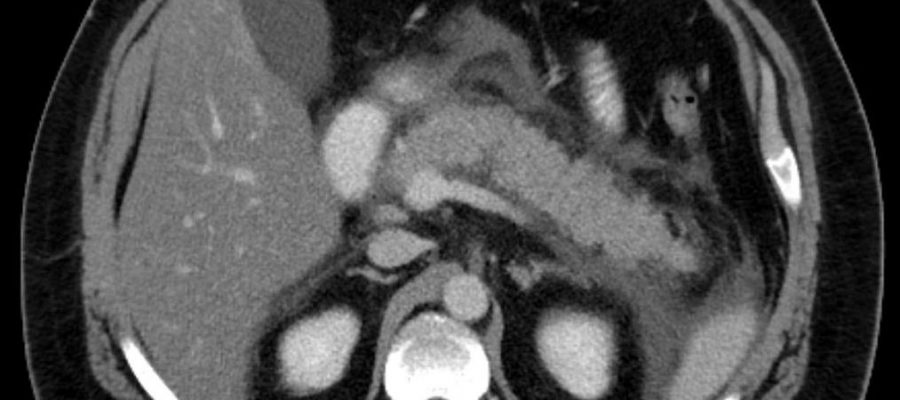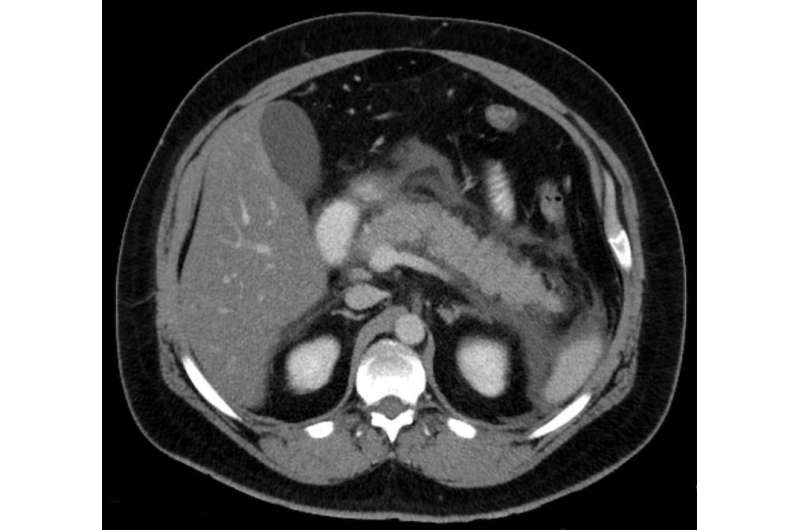
Pancreatitis is inflammation of the pancreas. The pancreas is a long, flat gland that sits tucked behind the stomach in the upper abdomen. The pancreas produces enzymes that help digestion and hormones that help regulate the way your body processes sugar. Pancreatitis occurs when digestive enzymes become activated while still in the pancreas, irritating the cells of your pancreas and causing inflammation.
Each year, about 275,000 hospital stays for acute pancreatitis and 86,000 hospital stays for chronic pancreatitis occur in the U.S., according to the National Institute of Diabetes and Digestive and Kidney Diseases.
Pancreatitis can occur as acute pancreatitis—meaning it appears suddenly and lasts for days. Some people develop chronic pancreatitis, which is pancreatitis that occurs over many years. Mild cases of pancreatitis improve with treatment, but severe cases can cause life-threatening complications, such as kidney failure, diabetes and pancreatic cancer.
Signs and symptoms of pancreatitis can vary, depending on which type you experience. Acute pancreatitis can cause upper abdominal pain, which can radiate to your back; fever; and nausea and vomiting. Chronic pancreatitis also can cause upper abdominal pain; as well as unexplained weight loss; and oily, smelly stools, called steatorrhea.
Factors that increase your risk of pancreatitis include:
• Excessive alcohol consumption: Research shows that people who consume four to five alcoholic drinks a day are at increased risk of pancreatitis.
• Cigarette smoking: Smokers are on average three times more likely to develop chronic pancreatitis, compared with nonsmokers. The good news is quitting smoking decreases your risk by about half.
• Obesity: You’re more likely to get pancreatitis if you’re obese.
• Diabetes: Having diabetes increases your risk of pancreatitis.
Source: Read Full Article