Billy Connolly discusses his struggles with alcoholism
We use your sign-up to provide content in ways you’ve consented to and to improve our understanding of you. This may include adverts from us and 3rd parties based on our understanding. You can unsubscribe at any time. More info
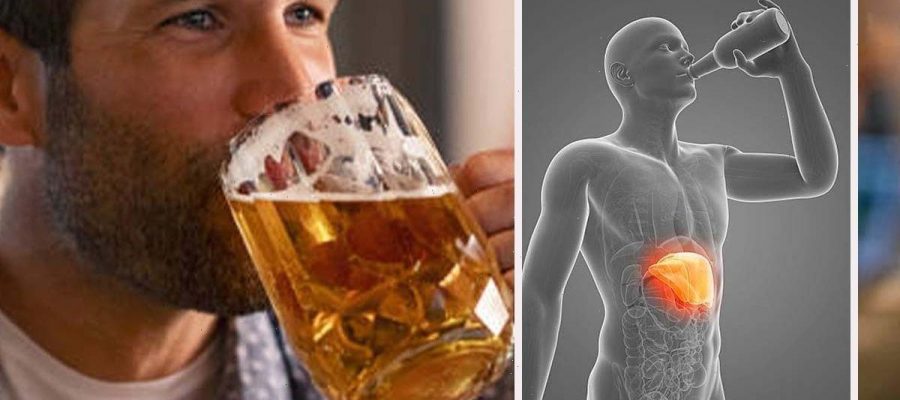
The British Liver Trust says: “ You don’t have to be addicted to alcohol to develop the condition, regularly drinking over the guideline amounts can put you at risk.” It says alcohol consumption is the most common cause of liver disease in the UK, accounting for six in 10 cases of liver disease. It adds up to one in five [people in the UK drink alcohol in a way that could harm their liver.
The Trust says you don’t have to show signs of addiction to be affected by alcohol-related liver disease and having half a bottle of wine or a few pints most evenings can damage your liver.
It states: “Generally, the more alcohol you drink above the recommended limits, the higher your risk of developing alcohol-related liver disease. It can make other types of liver disease worse too.”
The organisation explains: “It’s not only dependent or daily drinkers who develop liver disease. Heavy drinking even on a few days in the week can cause alcohol-related liver disease.
“It’s a lot easier to overdrink than many people realise, putting vast numbers of us in danger of alcohol-related illnesses.”
The Trust adds that these are the safer drinking limits are the same for men and women:
- Drink no more than 14 units a week
- Spread your drinking out over several days
- Have two to three days without alcohol every week, it’s best if they’re next to each other.
The NHS says symptoms of ARLD can include:
- Feeling sick
- Weight loss
- Loss of appetite
- Yellowing of the eyes and skin (jaundice)
- Swelling in the ankles and tummy
- Confusion or drowsiness
- Vomiting blood or passing blood in your stools.
The health body advises that if you regularly drink alcohol to excess, tell your GP so they can check if your liver is damaged.
The British Liver Trust says if you have any of these symptoms, tell a doctor straight away:
- Yellowing of the skin and whites of the eyes (jaundice), this can be harder to see if you have black or brown skin
- Tummy (abdominal) pains over the liver area
- Itching
- Losing a lot of weight for no reason
- Weakness and wasting of your muscles
- Swelling in the legs, ankles and feet caused by a build-up of fluid (oedema)
- Swelling in your tummy caused by a build-up of fluid (ascites)
- A tendency to bleed and bruise more easily, such as frequent nosebleeds and bleeding gums
- Periods of confusion, forgetting things, mood changes or poor judgement (encephalopathy or brain fog).
Cirrhosis is the most serious stage of alcohol-related liver damage, when the liver has a lot of severe scarring, and the charity says up to one in five heavy drinkers will develop cirrhosis.
The NHS explains that although the liver is very resilient and capable of regenerating itself. Each time your liver filters alcohol, some of the liver cells die.
It says: “The liver can develop new cells, but prolonged alcohol misuse (drinking too much) over many years can reduce its ability to regenerate. This can result in serious and permanent damage to your liver.”
The NHS says if you think you may need help with alcohol, a good place to start is with a GP. Try to be accurate and honest about how much you drink and any problems it may be causing you.
The health body explains: “The GP may suggest different types of assessment and support options available to you, such as from local community alcohol services.
“You can also ask about any free local support groups and other alcohol counselling that may suit you.”
It also says if you have become physically dependent and need to stop drinking completely, stopping overnight could be harmful. You should get advice about this and about any medicine you may need to do this safely.
If you’ve been regularly drinking over the guidelines for several months, it’s important to get your liver checked, it adds.
Source: Read Full Article